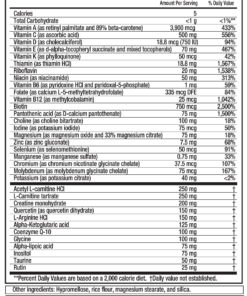
VITAMIN D (ALSO KNOWN AS VITAMIN D3 AND CHOLECALCIFEROL)
Vitamin D in EnergyNeeds®
 Vitamin D is added in order to provide a wide basis of nutrition. As EnergyNeeds® is designed to be used by a wide variety of individuals regardless of supplement status, the vitamin D dose in this product is high, but not among the very high doses advocated by some experts. Side effects and/or levels above the “normal” range are unexpected with the dose of vitamin D used in EnergyNeeds®. You may wish to speak to your physician regarding blood testing and potential additional vitamin D supplementation beyond that provided by EnergyNeeds®.
Vitamin D is added in order to provide a wide basis of nutrition. As EnergyNeeds® is designed to be used by a wide variety of individuals regardless of supplement status, the vitamin D dose in this product is high, but not among the very high doses advocated by some experts. Side effects and/or levels above the “normal” range are unexpected with the dose of vitamin D used in EnergyNeeds®. You may wish to speak to your physician regarding blood testing and potential additional vitamin D supplementation beyond that provided by EnergyNeeds®.
The Details
What Is vitamin D?
While the term vitamin D refers to a group of fat-soluble steroids, the most important member of this group, and the one present in supplements, is vitamin D3 (also known as cholecalciferol), which is referred to herein as simply “vitamin D”. Vitamin D can be synthesized in the skin from cholesterol through a process that is dependent on sun exposure to ultraviolet (UV) B radiation. Vitamin D is converted in the liver to 25-hydroxyvitamin D (also known as 25-OH-vitamin D), which is the compound measured in blood to determine a person’s vitamin D status. 25-OH-vitamin D is further converted by the kidneys to form 1,25-dihydroxyvitamin D, which is the biologically active form of vitamin D.
What Does 1,25-dihydroxyvitamin D do?
1,25-dihydroxyvitamin D (also known as calcitriol) circulates as a hormone in the blood, and has a major role in promoting the healthy growth and remodeling of bone. In particular, calcitriol increases intestinal absorption of calcium, magnesium, and phosphate, as well as being required for bone growth and remodeling by bone cells (osteoblasts and osteoclasts). Calcitriol also has several other effects, including on cell growth, proliferation, and differentiation, calcium signaling, brain development, neurotrophic and neuroprotective actions, neurotransmission, synaptic plasticity, neuromuscular activity, immune function, reduction of inflammation, and regulation of gene expression. Vitamin D regulates about 3% of all of the about 25,000 genes in humans, including activating the TPH2 gene that synthesizes tryptophan in the brain (https://www.ncbi.nlm.nih.gov/pubmed/24558199).
What Does a Deficiency of vitamin D Appear as?
Deficiency of vitamin D is caused by inadequate sun exposure in conjunction with inadequate dietary intake. Deficiency is increasingly common throughout the world. While often thought of as only a substantial issue in darker-skinned individuals, deficiency is common even among those the lightest skin tones with the modern custom of extensive skin coverage by clothes and sunscreens, and with increasingly sedentary indoor lifestyles. As vitamin D is present in appreciable quantities in only a few foods, mostly oily fishes and supplemented milk, supplementation is increasingly recommended. Of note, bowel disease can also predispose towards vitamin D deficiency by decreasing absorbance even when some supplementation is provided. Vitamin D deficiency typically results in impaired bone mineralization, which leads to bone fractures and bone-softening diseases including osteomalacia in adults, and rickets in children.
What About vitamin D’s Use in Disease?
Vitamin D is used for preventing and treating rickets, weak bones (osteoporosis), bone pain, bone loss in people with hyperparathyroidism, and inherited disorders causing weak bones such as osteogenesis imperfecta. It is also used for preventing falls and fractures in people at risk for osteoporosis, and preventing low calcium and bone loss in people with kidney failure. In addition, vitamin D is sometimes used for many conditions beyond bones, including high blood pressure, elevated cholesterol, diabetes, obesity, muscle weakness, autism, multiple sclerosis, rheumatoid arthritis, chronic obstructive pulmonary disease (COPD), asthma, bronchitis, premenstrual syndrome (PMS), tooth and gum disease, vitiligo, scleroderma, and psoriasis. Furthermore, some use vitamin D for boosting the immune system, preventing autoimmune diseases, and preventing cancer.
What Are the Common and/or Important Side Effects of vitamin D?
Vitamin D is fat soluble, yet toxicity appears to be rare, even in studies using extremely high doses such as 150,000 IU/month by intramuscular injection. Some sources suggest that blood levels of 25-hydroxyvitamin D above 50 or 60 ng/ml may be too high, and if present recommend reducing the amount of supplement provided (Institute of Medicine, Food and Nutrition Board. Dietary Reference Intakes for Calcium and Vitamin D. Washington, DC: National Academy Press, 2010; https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional). Side effects are rare at usual doses used in supplementation.
Is There Any Laboratory Testing for a Vitamin D Deficiency?
Blood testing of 25-hydroxyvitamin D is the best indicator of vitamin D status. Testing can be used to diagnosis deficiency as well as to monitor therapy, and often is recommended by many experts for individuals both in health and in disease.
What About Additional Dosing Beyond EnergyNeeds®?
EnergyNeeds® is designed to be used by a wide variety of individuals both healthy or with a wide range of disorders, many of which are already on vitamin D supplementation and/or with blood levels that already may have been determined to be adequate. In addition, there is a lot of controversy about what 25-hydroxyvitamin D levels are ideal, with the Institute of Medicine stating levels above 20 ng/ml are adequate (Institute of Medicine, Food and Nutrition Board. Dietary Reference Intakes for Calcium and Vitamin D. Washington, DC: National Academy Press, 2010), most laboratories listing 30 ng/ml as “normal”, and some studies recommending levels above 40 ng/ml. Achieving the latter level may require doses of which many physicians are uncomfortable. Thus, the vitamin D dose in this product (1,500 IU in adults) is high, but not among the very high doses advocated by some experts. You may wish to speak to your physician regarding blood testing and potential additional vitamin D supplementation beyond that provided by EnergyNeeds®.
Order EnergyNeeds® Today
Formulations